Innovations and projects
Cholangio.org innovations and projects collectively form a layered cholangiocarcinoma patient response system.
Cholangiocarcinoma is not only difficult because of its biology.
It is difficult because patients are often left without a clear pathway through it.
That is where time is lost.
And when time is lost, options are lost.
This is where the Foundation functions.
We do not focus on awareness.
We focus on what must be done now.
Today’s patient survival. Today.
Helping patients see what matters, early enough to act.
So they can act before those options are lost.
This work is delivered through defined projects.
Each project has a clear purpose, ownership, and role in improving survival.
Together, they form a patient-led survival system.
Cholangiocarcinoma is bile duct cancer.
If this is new to you, you can explore a simple explanation here.
The System Defined
The system behind the Foundation’s work.
The backbone from which every project is built.
Cancer operates as a system.
Response must operate as a system.
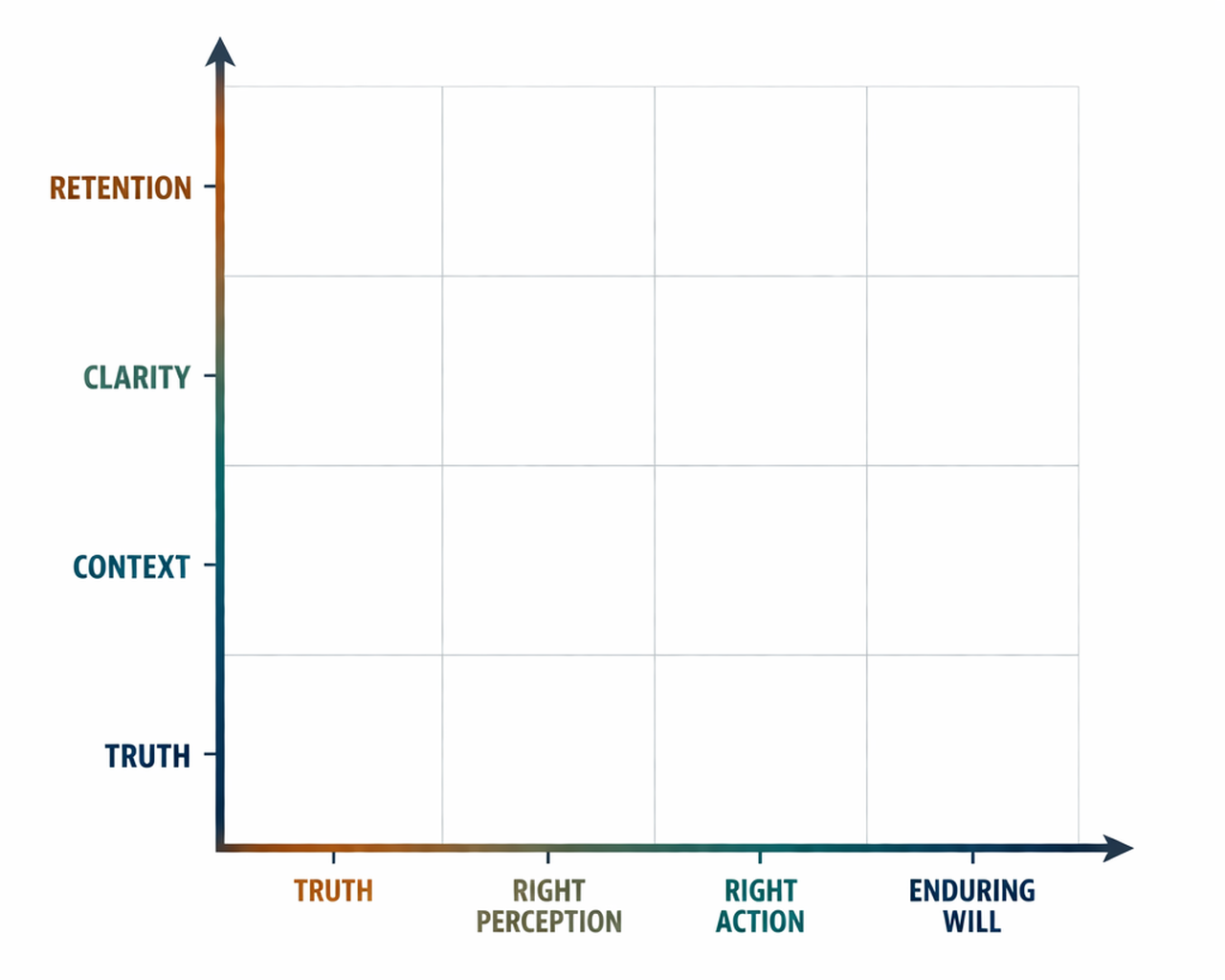
Biology → Physiology → Cognition
Truth is the axis.
Context → Clarity → Retention
Perception → Action → Will
Organised response → improved survival conditions
Innovations and projects
Core Infrastructure
Patient Response System
Journal. App. AI.
Patients shouldn’t be deprived of survival knowledge.
Most patients lose options not because of the cancer alone,
but because understanding comes too late.
We built the pathway to turn understanding into early action so that options won’t be lost.
The Patient Navigator Journal is how you start.
It is not a guide. It is a response system built from the lived experience of patients, caregivers, and clinicians.
It helps you know what to do, in the right order, when it matters most.
Description
Systemising biological and cognitive pathways.
Operationalises into a structured response for the patient.
The framework that structures how patients and clinicians move through the pathway of cholangiocarcinoma.
Converts the mapped terrain into a coordinated response system.
Problem This Resolves
Cancer care is delivered in disconnected phases.
Diagnosis and treatment are well addressed by the healthcare system.
The pathway between cause, diagnosis, treatment, and recurrence prevention is not.
Patients and families are left to navigate these gaps.
This fragmentation leads to delays, misalignment, and missed opportunities during critical decision periods.
Cholangiocarcinoma is not only difficult because of its biology.
It is difficult because the system around it is fragmented.
What the Project Does
The Optimal Patient Response Pathway serves a defined system function:
It builds the pathway.
It:
- Converts care into an informed and effective response
- Converts the biological and clinical terrain into a usable pathway
- Structures how patients and clinicians move through diagnosis and treatment
- Coordinates response across phases that are otherwise disconnected
- Establishes continuity across the full arc of the disease
- Reduces fragmentation within the system
It turns disconnected phases into a coordinated pathway patients and clinicians can move through together.
System Role
Within the survival system:
Truth → Pathway → Navigation → Learning → Alignment → Survival Culture
The Optimal Patient Response Pathway is the Pathway layer.
It defines the route.
The pathway defines the route.
The Patient Navigator Journal is how patients travel it.
Who It Serves
Patients, families, clinicians, and medical care teams moving through cholangiocarcinoma.
Current State
Operational within the Foundation’s patient response work.
Applied across patient cases and clinical collaboration.
What Funding Enables Next
Expansion of the pathway into scalable systems that support coordinated response across patients, clinicians, and care environments.
Development of tools and infrastructure that allow the pathway to be applied consistently across broader clinical networks.
Why This Matters
Survival is not shaped by treatment alone.
It is shaped by how effectively patients and clinicians move through the pathway between cause, diagnosis, treatment, and recurrence prevention.
Upgrading to:
Patient Response System
Journal. App. AI.
Patients shouldn’t be deprived of survival knowledge.
Most patients lose options not because of the cancer alone,
but because understanding comes too late.
We built the pathway to turn understanding into early action, so options won’t be lost.
The Patient Navigator Journal is how you start.
It helps you know what to do, in the right order, when it matters most.
Description
The Patient Navigator Journal is the navigation layer of the survival system where understanding becomes action.
It is the tool patients use to move through cholangiocarcinoma in a clear sequence, at the point where timing determines outcome.
Patients are not just given information.
They are guided step by step through what must be understood, decided, and done, in the order it must happen.
The Physical Journal:
- structures the early phase of response
- prepares patients for critical decisions
- translates complex biology into practical understanding
- aligns patients, families, and clinicians
- keeps action moving, so opportunities are not missed
This is not a guide. It is a response system in use.
Why is expansion required
The current Journal is effective but limited by format and reach.
Right now:
- Access depends on physical delivery
- Updates cannot move at clinical speed
- Reach is constrained, particularly outside major centres
This creates a delay, the exact problem the system is designed to solve.
System Evolution
The Patient Navigator Journal is evolving from a static guide into a responsive, adaptive system.
This expansion enables:
- Deeper patient orientation
New modules such as The Geography of Cholangio, help patients clearly see where they are in the disease and how it affects decisions - Clinical alignment at the patient level
National clinical guidelines are translated into clear, actionable patient understanding, reducing the gap between what should happen and what does happen - Integrated knowledge from lived experience
Insights from ongoing work, including The Book of Cholangio, strengthen how patients think, decide, and respond under pressure - AI-enabled navigation
The Journal evolves into an intelligent interface that can:
→ guide patients in real time
→ adapt to individual diagnosis and stage
→ surface what matters most, when it matters
→ reduce delay between diagnosis and effective action
What expansion enables
Expansion moves the Journal from a static tool to an interactive and responsive system.
- Digital Journal and app-based interface
- Immediate access at diagnosis, anywhere
- Real-time updates
- Clinical knowledge, pathways, and tools evolve without delay
- Integrated patient tools
- Biomarkers, questions, treatment pathways, and decision support in one place
- Wider distribution
- Reaching regional and underserved patients earlier
- Faster delivery
Reducing the time between diagnosis and a structured response
What this means in practice
Patients receive:
- earlier orientation
- clearer decisions
- better prepared consultations
- stronger alignment with their medical team
And most importantly, more time with options still available.
Close
Patients shouldn’t be deprived of survival knowledge.
Most patients lose options not because of the cancer alone,
but because understanding comes too late.
We are expanding the Patient Navigator Journal to ensure understanding comes early so action is taken in time, and options won’t be lost.
Description
The learning system that captures each patient journey and strengthens the pathway in real time.
Problem This Resolves
In most healthcare systems, patient experiences are not systematically captured or applied in real-time.
Lessons are lost between cases.
Knowledge does not accumulate in a structured way.
As a result, the pathway does not consistently improve.
What the Project Does
The Survival Intelligence System serves a defined system function:
It improves the pathway.
It:
- Captures patterns from patient journeys
- Identifies what improves response and what delays it
- Feeds those insights back into the pathway
- Strengthens navigation, decision-making, and timing for future patients
- It turns individual experience into system-wide learning.
System Role
Within the survival system:
Truth → Pathway → Navigation → Learning → Alignment → Survival Culture
The Survival Intelligence System is the Learning layer.
It ensures the pathway improves with every patient.
Who It Serves
All patients moving through the system, both now and in the future.
Current State
Active in early form through patient engagement, case observation, and pathway refinement.
Structured system development in progress.
What Funding Enables Next
Development of structured data capture, pattern recognition, and integration into pathway and navigation systems.
Expansion into a continuous learning infrastructure that improves response across all patient journeys.
Why This Matters
Without learning, the system repeats itself.
With learning, every patient strengthens the pathway for the next.
Description
Programs designed to improve patient access to advanced diagnostics, precision medicine, and emerging therapies.
Problem This Resolves
Many patients face delays or barriers in accessing genomic testing, targeted therapies, or clinical trials.
Access often depends on geography, financial capacity, or institutional pathways rather than patient need.
What the Project Does
The Foundation works to expand access to:
- genomic profiling
- precision medicine pathways
- specialist second opinions
- clinical trials
This helps patients reach specific cholangiocarcinoma treatment options earlier in their disease course.
- Increase response effectiveness
- Decrease time drift
- Remove or reduce unnecessary stress and
- cost outputs.
Who It Serves
Patients navigating diagnosis, treatment decisions, and clinical trial access.
Current State
A patient-led response system operating in parallel with clinical care.
- Every call is answered
- Every entry point is met with lived experience and structured guidance.
- Every referral is aligned with high-volume specialists experienced in cholangiocarcinoma.
What Foundation Funding Enables Next
Always-on access to lived experience and structured response support.
Scaled access programs that improve clinical selection and pathway alignment.
A coordinated national referral network directing patients to high-volume, cholangiocarcinoma-experienced centres.
Description
Unique Patient-Led Initiative
A mission-driven team environment comprised of patients and caregivers.
It activates lived experience and real-world capability to address gaps that delay or weaken patient response.
Teams are organised around defined projects and deployed where the system cannot move fast enough.
What it does
- Rapid response to patient needs
- Applies real capability under pressure
- Executes solutions that improve patient outcomes
- Focuses on execution, not awareness
Biological Intelligence & Research
Collaboration
Dr. Phillip Baird,
MB.BS, PhD(Syd), MHL(Syd), FRCPA. FIAC.
Pathologist – Cytopathologist
Description
Biological intelligence infrastructure that closes the causal and recurrence gap in cholangiocarcinoma response.
Problem this resolves
In current bile duct cancer care, bile is routinely discarded without formal observation or analysis.
As a result, biological cause and recurrence signals are lost, leaving diagnosis and treatment disconnected from the conditions that drive disease formation and return.
What the project does
Bile Bank collects and examines bile-related biological material that is otherwise lost to routine disposal.
It standardises observation, analysis, and longitudinal tracking of bile characteristics to restore visibility across causal pathways, treatment response, and recurrence risk.
Who it serves
Patients at risk of bile-related cancers, patients undergoing treatment, and survivors requiring ongoing recurrence monitoring.
Current state
Active. Foundational framework established.
What funding enables next
Expansion of collection protocols, analytical capacity, and integration of bile-derived markers into patient-facing monitoring and response systems.
Collaboration:
Together with the Cholangiocarcinoma Foundation Australia, Dr Ben Dwyer and his team at the Western Australian Organoid Innovation Hub and Liver Cancer Collaborative are working to personalise and improve treatment for bile duct cancer.
Description
A research initiative investigating how tumour biology may be influenced or redirected through environmental and systemic biological signals.
Using living tumour models grown from patients, we aim to help identify which therapies are most likely to work for each individual and understand the reasons underlying this response.
This work is designed to turn patient samples into biomarkers, new drug targets, and strategies to make cancers more vulnerable to therapy, accelerating progress toward more effective, tailored treatments for cholangiocarcinoma.
Problem This Resolves
Traditional oncology approaches focus primarily on destroying tumours after they emerge.
Less attention is given to understanding how the surrounding biological environment influences tumour behaviour and progression.
What the Project Does
This study explores mechanisms that influence tumour signalling and behaviour, with the goal of identifying pathways that may slow, redirect, or destabilise tumour growth.
It contributes to expanding treatment thinking beyond destruction toward biological influence and response modulation.
Who It Serves
Patients with active disease and researchers investigating new response strategies.
Current State
Early-stage research development.
What Funding The Foundation Enables Next
Early-stage collaboration, patient team and communications development, and early-stage cooperation with Ben and his team.
Clinical Standards
Collaboration
Prof John Zalcberg
MB BS, PhD, FRACP, FRACMA, FAICD
Head of Cancer Research Program, Monash University
Prof David Goldstein
MBBS, FRACP, PRCP (UK)
Conjoint Clinical professor and Senior Staff Specialist in the Department of Medical Oncology at Prince of Wales hospital in Sydney.
A/Prof Charles Pilgrim
MBBS, FRACS, PhD, FACS
Department of Surgery, Monash University.
General Surgeon, Hepatobiliary/Pancreatic Surgeon, Upper Gastrointestinal Surgeon
Description
The development of structured national guidance for cholangiocarcinoma diagnosis, treatment, and patient management.
Problem This Resolves
Cholangiocarcinoma remains a rare and complex cancer.
Clinical experience and treatment approaches vary significantly across institutions and regions.
This variability can delay optimal treatment decisions and limit patient access to emerging therapies.
What the Project Does
This initiative brings together clinicians, researchers, and patient leadership to define practical, evidence-informed guidance for managing cholangiocarcinoma across Australia.
The goal is to improve consistency in diagnosis, treatment sequencing, and patient referral pathways.
Who It Serves
Patients, clinicians, and health systems involved in cholangiocarcinoma care.
Current State
Development phase with clinical collaboration underway.
Manuscript “Controversies in the management of biliary tract cancer”
has been submitted to the ANZ Journal of Surgery by David Goldstein.
What Foundation Funding Enables Next
Patient-Led Integration of:
- National guidelines,
- development of community workshops and
- multi-state / major hospital symposiums
- participation in clinical review panels, and
- Patient-centred publication infrastructure
Explore the Full Pathway
- Understanding the disease
- How Win | Public Version of Cholangio OS
- Patient Navigator Journal
- Newly Diagnosed
PDF Cholangio.Org OS available on request
Contact claire@cholangio.org | +61 431180783
Where this fits
This article is part of a broader survival system developed through Cholangio.org.
Doctrines of Cholangio
Developed by Steve Holmes
The biological and cognitive pathway
The foundational thinking behind the system
↓
Cholangio.org OS
OPR: Optimal Patient Response
Systemising biological and cognitive pathways
Operationalising a structured response
↓
How We Win
The public-facing interface of the OS system
Activating a patient-led survival response
↓
The Survival System
Discussion Paper: The framework driving the Foundation
Coordinating action across patients, caregivers, and clinicians
↓
The Three Survival Disciplines
Discussion Paper: The human interface
How a patient engages and responds within the system
Patient Response System
Journal. App. AI.
Patients shouldn’t be deprived of survival knowledge.
Most patients lose options not because of the cancer alone,
but because understanding comes too late.
We built the pathway to turn understanding into early action so that options won’t be lost.
The Patient Navigator Journal is how you start.
It is not a guide. It is a response system built from the lived experience of patients, caregivers, and clinicians.
It helps you know what to do, in the right order, when it matters most.
➤ Order your free Patient Navigator Journal



